This article originally appeared in Red Flag
The coronavirus outbreak tearing through Sydney and now regional New South Wales is testing the public healthcare system like nothing before it. Yesterday, the Australian Medical Association said that the public health system can’t manage the increasing caseloads.
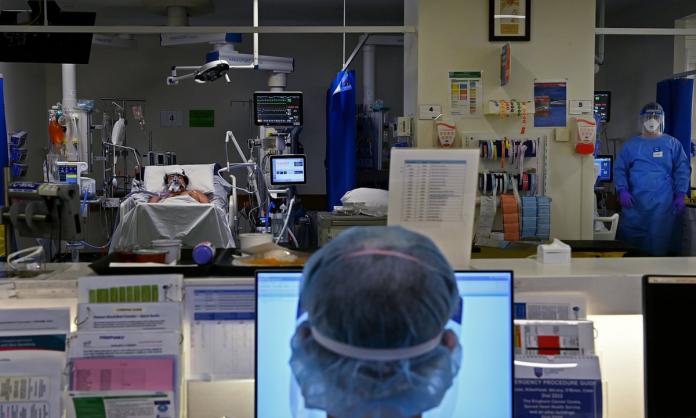
At my hospital in Sydney, there has been a complete upending of normal operations. Entire public wards have been moved into the private hospital, the intensive care unit has been expanded into the recovery unit, and entire floors have been turned into COVID-only wards. Nurses trained in anaesthetics are being given crash-courses in intensive care nursing; theatre nurses with little to no ward experience are being sent to look after geriatric COVID patients.
The hospital was not prepared for this outbreak. COVID patients are being transported in elevators and corridors that are used by the public—who are not wearing protective N95 masks—with only five or ten minutes between transports to allow for air circulation. This is super dodgy. It feels like it will be only a matter of time before patients and staff are infected, as happened at Liverpool Hospital. My hospital—indeed, all hospitals—are totally ill-equipped to deal with an outbreak of an airborne virus. A Victorian Department of Health report found that, during Melbourne’s second wave last year, 277 hospital patients caught the virus. Of those, 85 people died. Any hospital with a significant number of COVID patients is unsafe for unvaccinated people right now.
Even before this outbreak, the situation in hospitals was dire. Emergency departments were shockingly crowded and nurses were under great stress. The weight of responsibility for a patient’s health and the time-critical nature of disease and pain constantly collides with a system that is underfunded, under-resourced, understaffed and bed-blocked. It is incredibly frustrating to work in such an environment. Feeling like you can’t help people because you don’t have the time or resources is awful.
Management expects us to be perfect workers, to make no mistakes, to document every single thing, to answer all the call bells and telephones, to meet KPIs and to do all of our compulsory education in our own time. This leaves many nurses blaming themselves for the systemic problems. It’s ironic that hospitals, which are supposed to be places of healing, are the sites of such stress, anxiety and physical and emotional strain for the people who work in them. (It’s because of this that the nurses’ union, the NSW Nurses and Midwives’ Association, was already campaigning to improve staffing levels, pay and working conditions. The campaign has been put on hold while we battle the virus.)
COVID coming on top of this situation poses not only a serious risk to anyone who may catch the virus, but also to those admitted to hospitals for other reasons (there are some 3 million admissions per year in New South Wales). The state has just under 600 intensive care beds, mostly in metropolitan Sydney. Many regional hospitals are not capable of dealing with a surge in intensive care patients. Often, very ill patients in regional hospitals or patients requiring major surgery are transported to the closest major hospital. In most cases, that is Sydney. It is unclear what would happen if covid were to take hold in regional NSW. Where will the staff come from to run the intensive care units? ICU-trained doctors and nurses don’t just fall from the sky. They take years to train properly.
The coming weeks and months could be an unfolding crisis for the New South Wales healthcare system. Beyond the death toll, which is the main thing that the media reports, there will be the hidden toll. There will be thousands of people languishing in pain and disability because their surgeries have been cancelled. There will be the essential and potentially life-saving diagnostic procedures cancelled—leading to late diagnoses, and further preventable deaths. There will be the immeasurable toll of “long COVID” on hundreds of people. And then, if we manage to keep things relatively under control, there will be all of the catching up work.
One positive from the current outbreak is that far fewer people are dying than during Melbourne’s second wave. This is due to the high number of older people who have been vaccinated. Just one dose of any vaccine protects greatly against severe illness.
However, the Berejiklian government wants to gamble with our lives by easing restrictions once six million doses have been administered. To be clear, six million is a random number, chosen because it sounds big and is achievable even with the limited supply of vaccines. The population of New South Wales is eight million, and people require two doses, meaning that a 90 percent vaccination rate—which many epidemiologists are saying is needed for something approximating herd immunity against Delta—will require more than 14 million shots. Six million is a dangerously low target.
Eventually, restrictions will have to be eased, as it is widely believed that COVID is now endemic. Almost every epidemiologist acknowledges this. But easing restrictions when people have not even had a chance to be fully vaccinated is criminal. It is handing out death sentences to people, in the interests of business owners who want to begin trading as soon as possible. And it will likely push an already overloaded health system further into crisis.
The blame for this current outbreak, and the resulting death and damage to lives should be laid squarely at the feet of the Berejiklian government. For its refusal to follow the health advice. For its devotion to the interests of business. And for its years-long neglect of the public healthcare system and its workers.